MOVING HEALTH FORWARD
DHG supports efforts to move health forward by delivering innovative and leading
solutions for individuals whose lives are impacted by reduced movement.
Moving Health Forward
PRESSURE Ulcer Prevention
Intelligent Pressure Care
Moving Health Forward
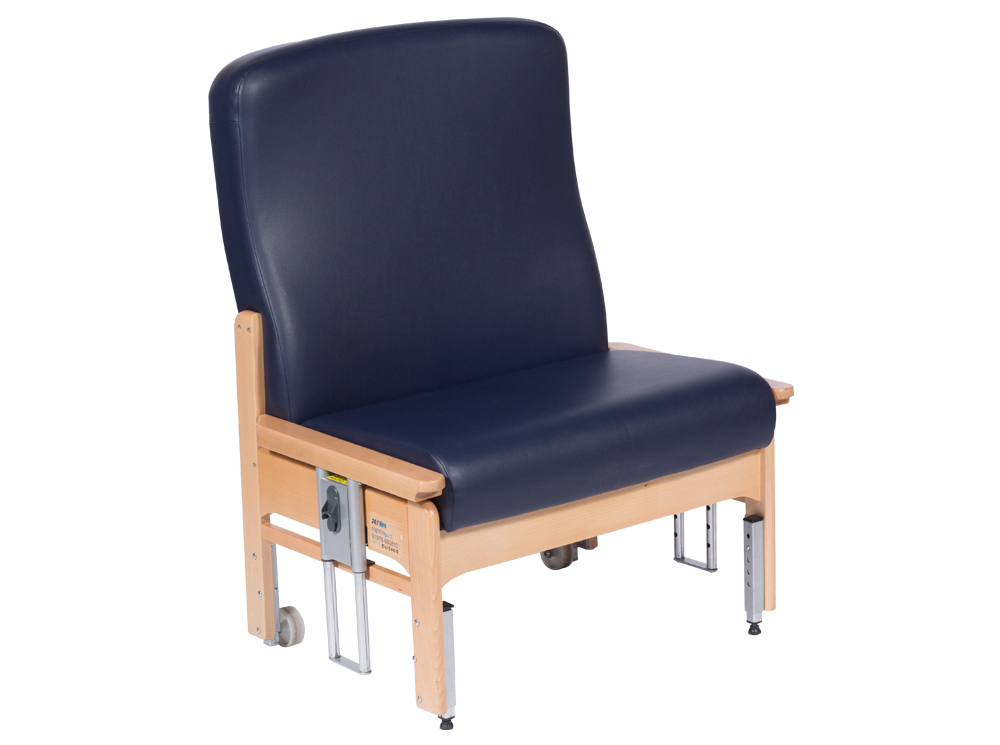
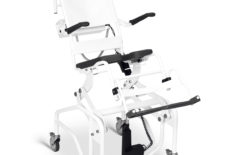
SPECIALIST SEATING
For Patients with Complex Care Needs
DHG
DHG strive to constantly support our healthcare partners, and the people whose healthcare needs they serve.
We work to keep improving the vital connections between movement and health,
enabling accelerated recovery and healthy independence in daily living.
Our Products
-
PRESSURE ULCER PREVENTION
-
Specialist Seating
-
Rental & Service Solutions
-
Safe Moving & Handling
-
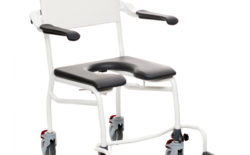
Bathroom Safety
Leader in the health application of pressure care technologies
Specialist seating solutions for patients with complex care needs
Rental & service care management solutions
Safe Moving & Handling solutions
Bathroom safety solutions